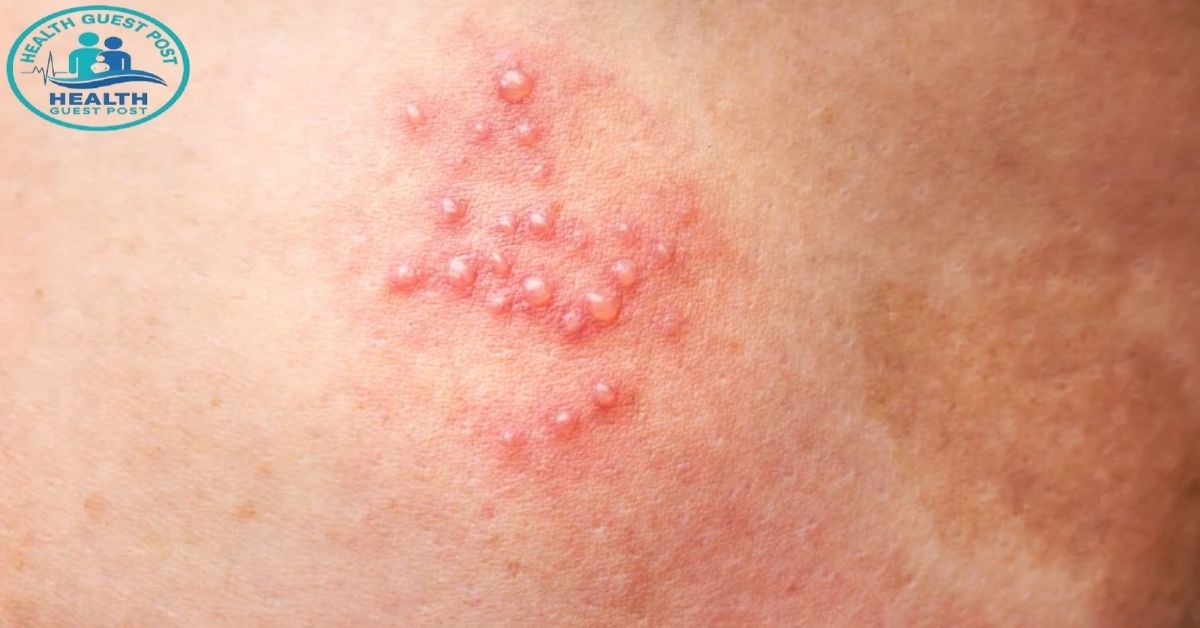
You noticed something unusual down there. Maybe a small bump, a sore, or some irritation you can’t explain. Your first thought might be panic. Your second might be denial. But here’s the thing: catching these signs early can genuinely change the outcome. Sexually transmitted infections affect millions of people every year, and many of them show up first as skin changes you can actually see. Knowing what to look for puts you ahead of the curve.
What are STD bumps?
STD bumps are skin lesions, sores, or unusual growths that appear as a result of sexually transmitted infections. They can show up on the genitals, inner thighs, mouth, or even the tongue depending on the type of infection involved. Some look like tiny pimples. Others resemble blisters, warts, or open sores. A few don’t hurt at all, which is exactly what makes them easy to ignore.
STD bumps are not all the same. Different infections cause different types of skin changes. Genital herpes tends to produce painful blisters that crust over. HPV, on the other hand, causes cauliflower-like genital growths that are usually painless. Syphilis can cause a single firm sore called a chancre. Molluscum contagiosum produces small, round, flesh-colored bumps with a dimple in the center.
The location matters too. Bumps in the genital area related to an STD are most commonly associated with herpes, HPV, or syphilis. But oral HPV bumps on the tongue or inside the mouth are more common than most people realize. If you’ve had unprotected oral contact, that’s a risk factor worth knowing about.
Signs of STDs to watch out for
Not every STD announces itself loudly. Some infections sit quietly for weeks or even months before showing any signs at all. That’s what makes awareness so important. Here are the genital infection warning signs you should never brush off.
Unusual bumps or sores anywhere on or near the genitals, mouth, or anus deserve attention. Itchy bumps caused by STDs often get mistaken for razor burn or ingrown hairs, especially in people who shave regularly. Vaginal itching and irritation that doesn’t go away on its own is another red flag. Penile discharge symptoms, particularly when combined with burning during urination, strongly suggest an infection like gonorrhea or chlamydia. An STD rash that spreads across the body, including the palms of the hands and soles of the feet, is a classic sign of secondary syphilis.
In short, if something feels off, looks different, or hasn’t cleared up within a few days, it’s time to get tested. Denial helps no one here.
Read More: Abdominal Muscle Strain Symptoms: How to Tell It’s a Pulled Stomach Muscle
What do herpes sores look like?
Herpes sores are one of the most searched topics when it comes to STI-related skin lesions, and for good reason. Genital herpes sores typically begin as small red bumps or tiny blisters. They cluster together, often appearing in groups. Within a day or two, those blisters burst and leave shallow, painful ulcers that can take one to four weeks to heal during a first outbreak.
The herpes blisters appearance changes depending on the stage. Early on, the skin might just feel tingly or itchy before anything shows up visually. That prodrome phase is actually a key identifier. Once the blisters form and break open, the raw sores can be quite painful. They eventually crust over and heal, but the virus stays in your body permanently.
Oral herpes, caused by HSV-1, often looks like cold sores around the lips or inside the mouth. The difference between herpes and HPV bumps is fairly clear once you know what to look for. Herpes causes painful, fluid-filled blisters that break open. HPV causes painless, rough, cauliflower-like growths. They feel different, look different, and behave differently.
Early symptoms of STD in females
For women, the early symptoms of STDs in females can be deceptively subtle. Vaginal discharge that changes in color, smell, or texture is often the first clue. Unusual spotting between periods sometimes points to chlamydia or gonorrhea. Pelvic pain or discomfort during sex can also signal an underlying infection.
Itchy bumps, irritation, or painful genital sores in and around the vaginal area are more visible signs. Some women notice a burning sensation while urinating, which is frequently associated with gonorrhea or a urinary complication from another STD. Swelling of the vulva or labia, combined with redness, is another sign that something’s off.
STD symptoms in women are often mistaken for yeast infections or bacterial vaginosis. That mix-up leads to delays in proper treatment. If over-the-counter treatments aren’t working, please see a doctor. A simple test can clarify everything.
Male STD warning signs
Men tend to notice STD symptoms differently. Warning signs of STDs in males often start with penile discharge, which can be white, yellow, or greenish depending on the infection. Burning during urination is a common companion symptom. Swelling or pain in the testicles can sometimes point to epididymitis caused by chlamydia or gonorrhea.
STD bumps on the shaft, head, or base of the penis are often the most visible sign. They might be small and painless, like warts, or they could be clustered blisters that signal herpes. A sore on the tip or around the foreskin that doesn’t heal within two weeks is worth taking seriously.
STD symptoms in men can also include a rash on the body, swollen lymph nodes in the groin area, or general fatigue. These broader symptoms often point to syphilis or HIV in its early stages. Don’t wait and hope they disappear on their own.
How to Treat STD Bumps?
The good news is that many sexually transmitted infections are treatable, and some are completely curable with the right approach. Here’s what treatment generally looks like.
Medications
Antiviral medications like acyclovir or valacyclovir are prescribed for herpes. They don’t cure the infection, but they reduce the frequency and severity of outbreaks significantly. Bacterial infections like chlamydia, gonorrhea, and syphilis are treated with antibiotics. Early-stage syphilis responds well to penicillin. Gonorrhea now requires dual antibiotic therapy due to growing resistance. HPV has no direct antiviral treatment, but its symptoms, meaning the warts and growths, can be removed through medical procedures.
Maintain Good Hygiene
Keeping the affected area clean and dry helps prevent secondary infections. Use mild, unscented soap and warm water. Avoid scrubbing sores, as that slows healing and increases pain. Wear loose, breathable cotton underwear to reduce friction and moisture buildup around any active sores or bumps.
General Care
Rest matters more than people think. Your immune system does a lot of the heavy lifting during an outbreak. Staying hydrated, eating well, and reducing stress all support faster recovery. Avoid sexual contact during active outbreaks to prevent spreading the infection to a partner.
Topical Treatments
For HPV-related warts, a doctor might prescribe imiquimod cream or podophyllin. These treatments work by stimulating the immune system or destroying the wart tissue directly. Never use over-the-counter wart removers on genital warts. The skin there is far more sensitive than the skin on your hands or feet, and the wrong product can cause serious irritation.
Never ignore the signs of STDs
Here’s the honest truth. STDs don’t always come with a neon sign. Sometimes it’s just an itchy bump. Sometimes it’s a sore that seems minor. But leaving these signs unaddressed creates real problems, including spreading the infection to others, developing complications like pelvic inflammatory disease, or in rare cases, increasing your risk for certain cancers linked to untreated HPV.
Knowing how to identify STD bumps, understanding when to see a doctor for STD bumps, and getting tested regularly are the three most powerful things you can do for your sexual health. Testing is quick, often free at clinics, and completely confidential. There’s no reason to sit on uncertainty when answers are so accessible.
Can STD bumps go away on their own? Sometimes, yes, especially with HPV in younger people whose immune systems clear the virus naturally. But that’s not a reason to skip the doctor. Get tested. Get clarity. Take action.
FAQ’s
What are STD bumps exactly?
They are skin sores, blisters, or growths caused by sexually transmitted infections like herpes, HPV, or syphilis. They vary in appearance depending on the specific infection.
What do STD bumps look like?
They can look like blisters, warts, open sores, or pimple-like bumps. Some are painful, others are completely painless, and they often appear in clusters.
Can STD bumps appear on the tongue?
Yes. Oral HPV symptoms can cause bumps or warts inside the mouth and on the tongue, especially after unprotected oral sex.
How do I know if a bump is an STD or something else?
You can’t always tell by looking. A medical professional can test and confirm the cause. Don’t self-diagnose based on appearance alone.
When should I see a doctor for genital bumps?
See a doctor if a bump doesn’t heal within two weeks, is painful, spreads, comes with discharge or fever, or appears after unprotected sexual contact.

Liam Grant is a health writer passionate about evidence-based wellness. With a background in nutrition and digital health research, he shares practical, medically reviewed insights promoting balanced living. Evan’s work focuses on trustworthy, expert-backed health advice designed to improve daily habits, mental clarity, and overall well-being for readers worldwide.