Have you ever felt so short of breath that even lying down felt like a struggle? Or woken up in the middle of the night gasping for air? These aren’t just random health scares. They could be signs of something serious happening inside your lungs and heart. Pulmonary vascular congestion is one of those conditions that often gets missed until it becomes a real emergency. And yet, catching it early can genuinely change the outcome.
This guide breaks everything down in plain, simple language. No overwhelming medical jargon. Just the facts you need, explained clearly so you can actually use them.
What is Pulmonary Vascular Congestion?
Let’s start with the basics. Your lungs are filled with a vast network of tiny blood vessels. These vessels carry blood in and out, exchanging oxygen and carbon dioxide with every breath you take. When everything works as it should, this process is smooth and effortless.
But sometimes, blood starts to back up inside those vessels. Pressure builds. Fluid leaks into the lung tissue. Breathing becomes harder. That’s pulmonary vascular congestion in a nutshell. It’s essentially a traffic jam inside your lungs’ blood vessels, and the consequences ripple outward fast.
This condition is closely linked to congestive heart failure, particularly left-sided heart failure. When the left side of your heart can’t pump blood efficiently, blood pools in the pulmonary veins. That pooling raises pressure in the lungs and triggers the entire cascade of symptoms that make this condition so dangerous. It’s not a standalone disease. It’s usually a signal that something bigger is going wrong upstream, often in the heart itself.
Read More: IV for Dehydration: When You Need Hydration
Pulmonary Vascular Symptoms
The tricky thing about this condition is that its symptoms can sneak up on you. They often start mild and get dismissed as tiredness or a minor chest issue. But over time, they intensify.
Shortness of breath is the most common and noticeable symptom. You might feel it during light activity at first, then even while resting. Fatigue hits differently here too. It’s not just feeling tired after a long day. It’s a deep, persistent exhaustion that doesn’t go away with rest.
Coughing is another red flag, especially a persistent cough that produces frothy sputum. That foamy mucus is a telltale sign that fluid has started leaking into the airway. Chest tightness is common as well, and many people describe it as a pressure or heaviness sitting right in the middle of the chest.
One particularly telling symptom is paroxysmal nocturnal dyspnea. That’s a fancy term for waking up suddenly at night, unable to breathe properly. It happens because when you lie flat, fluid redistributes in the lungs, making breathing even harder. People with this symptom often find themselves sleeping propped up on multiple pillows just to breathe comfortably.
Peribronchial thickening, something often spotted on a chest X-ray, is another indicator that the airways are under pressure from surrounding congested tissue. Swollen ankles, reduced urine output, and even confusion in severe cases can also appear as the body struggles to compensate for oxygen deficiency.
Pulmonary Vascular Congestion vs Pulmonary Hypertension
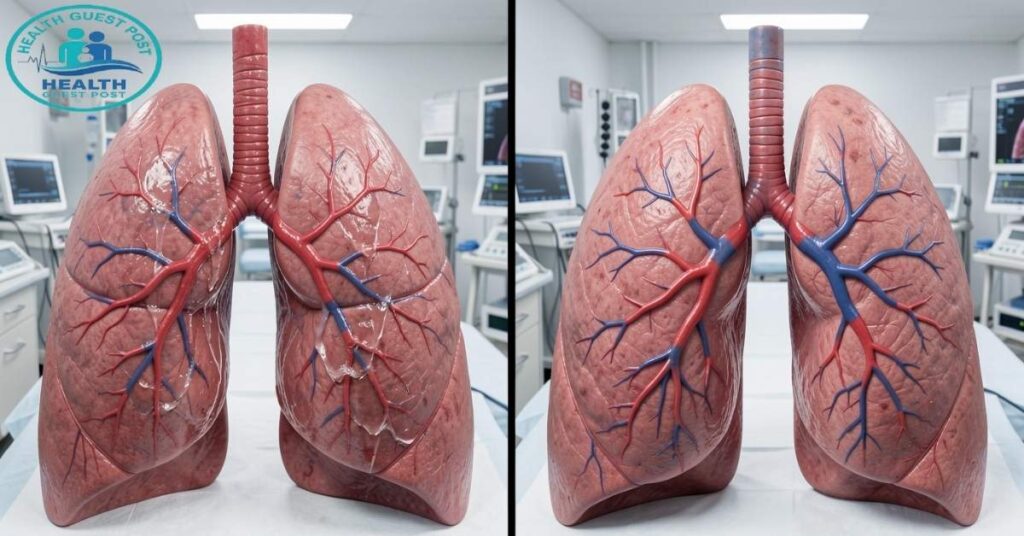
People often confuse these two conditions, and honestly, it’s understandable. They both involve abnormal pressure in the lungs’ blood vessels. But they’re not the same thing, and the distinction matters a lot when it comes to treatment.
Pulmonary vascular congestion is typically caused by a backup of pressure from the left side of the heart. The problem originates downstream, in the heart, and the lungs bear the consequences. It’s reactive. The lung vessels aren’t the root of the problem but rather the victims of it.
Pulmonary hypertension, on the other hand, is defined by persistently high pulmonary artery pressure. In many cases, the disease originates within the pulmonary vessels themselves. The arteries thicken, narrow, and become stiff over time. This increases resistance in the lungs and forces the right side of the heart to work much harder.
Both conditions can cause dyspnea, fatigue, and reduced exercise tolerance. Both show up on an echocardiogram as elevated pressures. But their causes, progressions, and treatment paths diverge significantly. Treating pulmonary hypertension with diuretics alone, for instance, won’t address the underlying vascular changes. Knowing which condition you’re dealing with is step one in getting the right care.
Classification of Pulmonary ICD-10
Medical coding might sound dry, but it’s actually important for how doctors document, bill, and track your condition. ICD-10 is the International Classification of Diseases, 10th edition. It gives every diagnosed condition a specific code. These codes guide treatment decisions, insurance coverage, and medical records.
For pulmonary conditions involving vascular congestion, fluid accumulation in lungs, or related heart failure complications, accurate ICD-10 coding ensures you get the right care pathway from the start.
Learn about the Common Pulmonary ICD-10 Codes
There are several pulmonary ICD-10 codes that come up frequently in clinical settings. J81.0 refers to acute pulmonary edema, which is the severe, rapid form of fluid accumulation. J81.1 covers chronic pulmonary edema, a longer-lasting version of the same problem.
I50.1 is the code for left ventricular failure, which is closely tied to pulmonary vascular congestion since left-sided heart failure is one of its primary drivers. I27.0 covers primary pulmonary hypertension, while I27.2 is used for other secondary forms of pulmonary hypertension.
For hypertensive heart disease with heart failure, I11.0 is the relevant code. Ischemic heart disease codes, like I25.10, may also appear in records when coronary artery disease is contributing to the heart’s reduced pumping ability. These codes matter because they shape how your condition gets managed in the healthcare system. A wrong code can mean delayed treatment or denied coverage.
What is Pulmonary Vascular Congestion Life Expectancy?
This is the question that weighs on every patient and family member. And the answer, while not simple, carries genuine hope when treatment is pursued early.
Life expectancy in pulmonary vascular congestion depends heavily on the underlying cause. If congestive heart failure is driving it, the outlook varies based on the stage of heart failure, how well it responds to treatment, and whether other conditions like kidney disease or hypertensive heart disease are in the picture.
Studies show that patients with well-managed heart failure can live for many years after diagnosis. The key phrase there is “well-managed.” When blood pressure control is optimized, medications are taken consistently, and lifestyle changes are made, the trajectory improves substantially. Early symptom detection plays a massive role here.
On the flip side, untreated or poorly managed pulmonary vascular congestion can lead to rapid deterioration. Repeated hospitalizations, progressive fluid overload, and organ strain can cut life expectancy significantly. Patients with advanced stages who do not respond to standard treatments may face a more limited prognosis, typically within one to three years.
But here’s what matters most: no two patients are the same. Age, overall health, responsiveness to treatment, and access to advanced cardiac therapies all factor in. Talking openly with your cardiologist about your specific situation gives you the clearest picture.
Pulmonary Vascular Causes
Understanding what causes this condition helps you make sense of why it develops and what can be done about it. The most common culprit is left-sided heart failure. When the left ventricle loses its pumping power, blood backs up into the pulmonary veins, pressure rises, and fluid begins leaking into the lung tissue.
Heart valve disease is another significant cause. A faulty mitral valve, for instance, can prevent blood from flowing forward properly, sending it back into the lungs instead. Ischemic heart disease, where reduced blood supply damages the heart muscle, can weaken the heart to the point where it can no longer manage normal circulatory demands.
Hypertensive heart disease is a major contributor too. Chronically high blood pressure forces the heart to pump harder against resistance. Over time, this strains and thickens the heart muscle, impairing its function. Lung infection and pneumonia can also trigger acute episodes of congestion, especially in patients who already have underlying cardiac issues.
Kidney disease adds another layer of complexity. When kidneys can’t excrete enough fluid, it builds up in the body, including the lungs. Pulmonary vascular leak, where the vessel walls become abnormally permeable, also contributes to fluid accumulation. Even certain medications or toxin exposure can trigger pulmonary vessel dilation and subsequent congestion.
Pulmonary Vascular Congestion Treatment
The good news is that this condition is treatable. The approach depends on se
verity, underlying cause, and how the patient responds. Let’s walk through the main treatment options.
Medications
Diuretics are often the first line of defence. They help your body flush out excess fluid through urine, reducing the fluid overload in the lungs. Furosemide is one of the most commonly used. ACE inhibitors and beta-blockers are frequently prescribed to reduce the heart’s workload, lower blood pressure, and improve cardiac function over time.
For patients with atrial fibrillation or blood clot risk, anticoagulants may be added. Vasodilators help by relaxing and widening the blood vessels, reducing the resistance the heart has to pump against. In cases where infection is driving the congestion, appropriate antibiotics are prescribed to tackle the underlying lung infection directly.
Oxygen Therapy
When oxygen deficiency becomes a concern, supplemental oxygen therapy is introduced. It helps maintain adequate oxygen levels in the blood while the underlying cause is being treated. In severe acute cases, patients may require high-flow oxygen or even ventilatory support.
Oxygen therapy doesn’t fix the root problem, but it buys time and reduces strain on the heart and organs during the most critical phase of treatment.
Treating the Cause
This is arguably the most important step. Managing the condition that’s driving the congestion is what creates lasting improvement. If left-sided heart failure is the cause, optimizing heart failure management is central. If heart valve disease is involved, surgical repair or replacement of the valve may be necessary.
For patients where hypertensive heart disease is the driver, achieving consistent blood pressure control through medication and lifestyle changes is critical. Addressing kidney disease, managing infections, and adjusting contributing medications all fall under this umbrella too.
Advanced Therapies
When standard treatments aren’t enough, more advanced options come into play. An implantable cardioverter-defibrillator (ICD) may be recommended for patients at high risk of dangerous arrhythmias alongside heart failure. Cardiac resynchronization therapy helps improve the coordination of the heart’s pumping chambers.
In end-stage cases, heart replacement through transplantation may be evaluated. EKG services and regular echocardiogram monitoring are used to track the heart’s function over time and guide treatment adjustments. Emergency care treatment protocols exist for acute episodes where rapid fluid removal and stabilization are needed.
Final Words
Pulmonary vascular congestion is serious. But it’s not a dead end. The more you understand it, the better equipped you are to take action. Whether you’re a patient navigating a new diagnosis, a caregiver supporting someone you love, or simply someone who wants to stay informed, knowledge is your most powerful tool here.
Catch the symptoms early. Get the right tests. Work with a specialist who knows your full health picture. And don’t ignore those midnight breathlessness episodes or that persistent cough. Your lungs are trying to tell you something. It’s worth listening.
FAQ’s
What is the main cause of pulmonary vascular congestion?
The most common cause is left-sided heart failure, where the heart can’t pump blood forward efficiently, causing it to back up into the lungs and raise pressure in the pulmonary veins.
Can pulmonary vascular congestion be reversed?
In many cases, yes. With proper treatment of the underlying cause, including medications, fluid management, and lifestyle changes, significant improvement is possible and symptoms can reduce substantially.
How is pulmonary vascular congestion diagnosed?
Doctors typically use a chest X-ray, echocardiogram, and EKG services alongside blood tests and physical examination to confirm the diagnosis and identify the underlying cause.
Is pulmonary vascular congestion the same as pulmonary edema?
They are closely related but not identical. Pulmonary edema refers specifically to fluid accumulation in the lung tissue, while pulmonary vascular congestion is the broader process of increased pressure and fluid buildup within the lung’s blood vessels.
What lifestyle changes help manage this condition?
Reducing salt intake, monitoring fluid intake, staying active within safe limits, avoiding smoking, maintaining a healthy weight, and keeping up with all prescribed medications are all highly beneficial for managing this condition long-term.

Liam Grant is a health writer passionate about evidence-based wellness. With a background in nutrition and digital health research, he shares practical, medically reviewed insights promoting balanced living. Evan’s work focuses on trustworthy, expert-backed health advice designed to improve daily habits, mental clarity, and overall well-being for readers worldwide.