You push hard during training. Your foot starts aching, not the usual soreness, but something that lingers even after rest. You brush it off. A week later, you can barely put weight on it. Sound familiar? That nagging pain might not just be fatigue. It could be a hairline fracture in foot, one of the most underestimated and under-diagnosed injuries in the athletic world.
These tiny bone cracks don’t announce themselves loudly. They creep up on you. And if ignored, they can sideline you for months. Whether you’re a marathon runner, a weekend basketball player, or someone who just ramped up their walking routine, understanding stress and hairline fractures can genuinely protect your long-term bone health.
What Is a Stress or Hairline Fracture?
Most people picture a fracture as a dramatic snap, a bone that breaks clean in two from a single traumatic force. But stress and hairline fractures don’t work that way. They’re quieter. More deceptive. And in many ways, more dangerous because of that.
Understanding Small Bone Cracks
Your bones are living tissue. They constantly break down and rebuild through a process called bone remodeling. Under normal circumstances, your body keeps that cycle balanced. But when you repeatedly load the same bone beyond its ability to recover, especially without adequate rest, microscopic damage accumulates faster than the bone can repair itself. The result is a microfracture, a tiny crack that develops from the inside out.
Think of bending a paper clip back and forth. It doesn’t snap on the first bend. It weakens gradually until one day it gives. Your bones work similarly under repetitive stress. The crack starts small, often invisible to the naked eye, but it’s real and it hurts.
These small bone cracks are extremely common in weight-bearing bones, particularly in the feet, shins, and ankles. Runners and athletes who engage in high-impact sports experience them at disproportionately high rates.
Stress Fracture vs. Hairline Fracture
Here’s where many people get confused, and honestly, it’s an easy mix-up. The terms “stress fracture” and “hairline fracture” are often used interchangeably, and in clinical settings, they often refer to the same type of injury. But there are subtle distinctions worth knowing.
A stress fracture is specifically caused by repetitive mechanical loading over time. It’s the product of overuse. An athlete who increases training intensity too quickly, without allowing adequate bone recovery time, develops a stress fracture. It’s an overuse injury at its core.
A hairline fracture, technically speaking, refers to the physical appearance of the crack, a thin, hair-like line visible on imaging. It can result from repetitive stress or even from a single moderate impact on a bone that’s already weakened. So all stress fractures may appear as hairline fractures on imaging, but not all hairline fractures are caused by stress alone. The distinction is subtle, but it matters when pinpointing the underlying cause and planning treatment.
Read More: Pulled Chest Muscle: Symptoms, Causes, Treatment & When to Seek Emergency Care
Types of Fractures in Athletes and Active Individuals
Not all stress fractures feel the same or heal the same. Where the crack occurs changes everything, the symptoms you feel, how long recovery takes, and how aggressively it needs to be managed.
Foot Stress Fractures (Metatarsals)
The metatarsal bones are the long, slender bones in the middle of your foot connecting your ankle to your toes. They absorb an enormous amount of force with every step. Metatarsal fractures are among the most frequent stress injuries in runners, dancers, and military recruits. The second and third metatarsals are particularly vulnerable due to their mechanical load-bearing role.
Pain typically concentrates on the top of the foot and worsens with activity. You might notice swelling around a specific spot rather than diffuse foot pain. This localized tenderness is a classic red flag. Hairline fracture in foot injuries affecting the metatarsals often go undetected on initial X-rays, making MRI the preferred diagnostic tool in ambiguous cases.
Shin Stress Fractures (Tibial)
Shin fractures are disturbingly common among distance runners. The tibia, being the primary weight-bearing bone of the lower leg, endures massive cumulative force over long runs. Tibial fractures can occur anywhere along the bone but are most frequently seen in the middle and distal thirds.
What makes tibial stress fractures tricky is how easily they mimic shin splints, a far less serious condition. Both produce pain along the shin, particularly during running. The key difference? Shin splints cause diffuse pain along a wider area, while a stress fracture produces sharp, focal tenderness at a precise point. Press your finger along your shin, if one specific spot makes you wince, that’s worth investigating.
Ankle Stress Fractures
Ankle stress fractures are less common than foot or shin injuries but can be particularly disruptive. The navicular bone and the fibula are the most frequent ankle structures affected. Navicular fractures are notoriously slow to heal due to poor blood supply, and athletes who delay treatment often face extended recovery.
The ankle instability that accompanies these fractures is frustrating. You’ll likely feel deep, diffuse pain around the ankle that doesn’t respond to typical sprain treatments. If you’ve been treating what seems like a chronic sprain for weeks without improvement, get imaging done.
Heel Stress Fractures (Calcaneal)
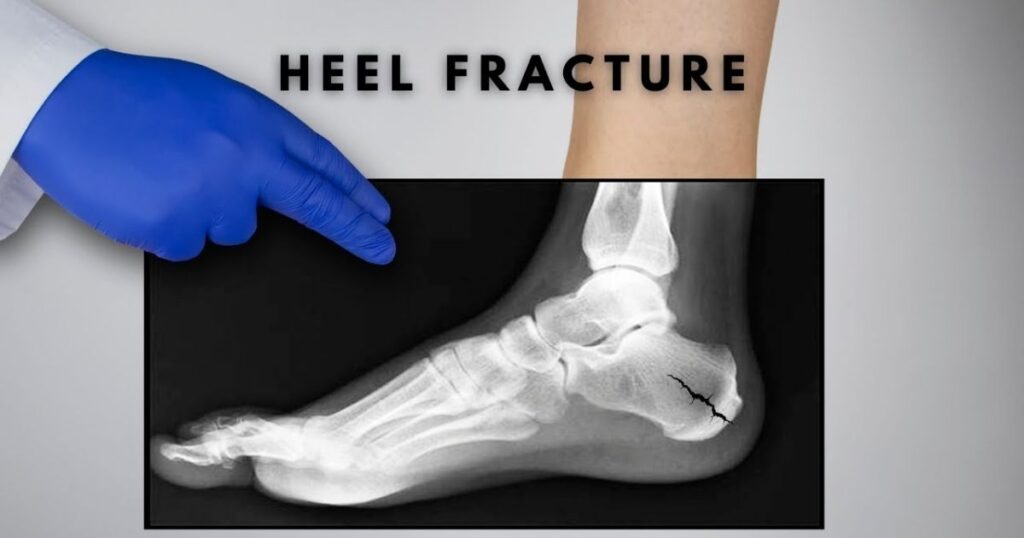
Calcaneal fractures affect the heel bone. They’re less common in runners but show up more frequently in military trainees and people who’ve recently started high-impact exercise after a long sedentary period. The pain is typically a stabbing heel pain that’s worst first thing in the morning or when resuming activity after rest, which makes it easy to confuse with plantar fasciitis.
One distinction: plantar fasciitis pain tends to ease as you walk and warm up. Heel stress fracture pain often persists or worsens with continued activity.
Leg and Other Less Common Fractures
Femoral stress fractures, while rare, are among the most serious. The femur, or thigh bone, is the strongest bone in your body. When it develops a stress fracture, that’s a sign of severe overtraining or a significant underlying bone density issue. These require prompt medical attention because a complete femoral break can be life-altering.
Fibula fractures, pelvic stress fractures, and even rib stress fractures (seen in rowers) round out the less typical but equally real forms of bone fatigue injuries.
Who Is at Risk of Developing Stress Fractures?
Stress fractures don’t discriminate entirely, but they do have favorite targets. Certain profiles carry significantly elevated risk.
Athletes, Runners, and High-Impact Sports
Distance runners top the list. The sheer repetitive loading involved in running, especially on hard surfaces, accumulates rapidly. A single mile of running generates thousands of foot strikes. Multiply that by five, ten, or twenty miles a week, and you start to understand why bones eventually protest.
Basketball players, gymnasts, soccer players, and military trainees are also at elevated risk. Any sport involving repeated jumping, pivoting, or long-distance movement puts stress on the same bone structures over and over. Running injury statistics suggest that stress fractures account for up to 20% of all sports medicine consultations.
Female Athlete Triad and Low Bone Density
This is a critical topic that doesn’t get enough attention. The female athlete triad refers to the combination of low energy availability (often from disordered eating), menstrual irregularities, and low bone density. Female athletes who restrict caloric intake to maintain a certain body weight or performance standard often develop hormonal disruptions that accelerate bone loss.
The result? Stress fractures at rates significantly higher than their male counterparts, even when performing the same training volumes. If you’re a female athlete experiencing irregular periods alongside recurring bone pain, that combination warrants a serious conversation with your healthcare provider. It’s not just about the fracture, it’s about long-term skeletal health.
Overtraining, Improper Footwear, and Sudden Activity Increases
You’ve probably heard of the “too much, too soon” principle. It’s real. The number one behavioral risk factor for stress fractures is a sudden spike in training volume or intensity without adequate progression. Your bone’s remodeling cycle takes weeks to adapt. Jumping from running 20 miles a week to 40 in a single training block simply doesn’t give bone tissue enough time to keep up.
Improper footwear compounds the risk considerably. Worn-out running shoes that no longer provide adequate cushioning transfer more force directly to your bones. Running in shoes designed for a different gait pattern or activity type adds biomechanical stress. Even something as simple as switching from grass to pavement without gradually adapting can trigger overuse injury in susceptible individuals.
Symptoms and Warning Signs of Stress Fractures
The tricky thing about stress fractures is that early symptoms are easy to rationalize away. “I’m just sore from training.” “I’ll feel better after a rest day.” Sometimes that’s true. But other times, that dismissal allows a small crack to become a larger problem.
Pain Patterns: Mild Ache to Sharp Pain
Early-stage stress fractures usually present as a dull, generalized ache during or after physical activity. You might not even notice it at first except on long runs or toward the end of a workout. As the fracture progresses, the pain becomes sharper, more localized, and starts appearing earlier in your activity. Eventually, it shows up at rest, too.
The pain typically follows a predictable pattern: mild at the start of activity, worsening as you continue, then easing somewhat when you stop, only to return with the next session, a little worse each time. Don’t ignore that escalating pattern.
Swelling, Tenderness, and Bruising
Localized swelling around the fracture site is a classic sign. Run your fingers along the affected bone. Is there a spot that feels puffier than the surrounding area? Is pressing on it sharply painful? That point tenderness at the fracture site is one of the most reliable physical indicators.
Bruising in severe cases can emerge a day or two after the fracture develops. It’s not always present, and its absence doesn’t rule out a fracture. But when bruising shows up alongside swelling and point tenderness, it strongly suggests something more significant than muscle fatigue.
Early vs. Progressive Symptoms
Early symptoms are subtle, easy-to-ignore aches that fade with rest. Progressive symptoms are harder to dismiss: pain that persists through the night, difficulty walking on flat ground, swelling that doesn’t subside, and tenderness that intensifies with even light pressure.
If you reach the progressive stage, you’ve likely been dealing with this for weeks. The bone has been trying to tell you something. At this point, professional evaluation isn’t optional, it’s urgent.
How Stress and Hairline Fractures Feel
Everyone experiences pain differently. But stress fractures do have fairly characteristic sensory signatures depending on where they occur. Knowing these can help you connect your specific symptoms to a potential diagnosis.
Foot and Ankle Sensations
A foot stress fracture sensation is often described as a burning or throbbing discomfort on the top of the foot, worsening with each footfall. Some people describe it as “stepping on a pebble” that never goes away. With ankle fractures, the sensation tends to be deeper, a persistent ache that feels almost like it’s coming from inside the joint rather than on the surface.
Many people initially mistake foot stress fractures for tendinitis or bursitis because the pain pattern can overlap. If topical treatments and stretching aren’t helping after a week or two, consider a different diagnosis.
Shin Pain and Heel Pain
Shin pain while running is one of the most common complaints in endurance sports. The challenge is distinguishing run-of-the-mill shin splints from a genuine tibial stress fracture. As mentioned earlier, the key is localization. Shin splints spread their discomfort across a wider section of the shin. A stress fracture hurts right there, at one specific spot.
Stabbing heel pain that’s worst with the first steps in the morning or after prolonged sitting can indicate calcaneal involvement. Unlike the diffuse tightness of plantar fasciitis, this pain often has a sharp, almost electric quality right at the heel bone.
Activity-Dependent Pain and Hop Test
Here’s something useful you can try at home. It’s called the hop test. Stand on the affected leg and hop once. If you feel a sharp, specific pain at the suspected fracture site, that’s a meaningful indicator. It’s not a diagnostic tool by itself, but it helps distinguish vague soreness from a genuine bone crack.
Keep in mind that pain during activity that resolves with rest, and consistently returns when you resume, is one of the clearest hallmarks of a stress fracture. It’s not random. It’s mechanical.
Diagnosis and Imaging for Fractures
You suspect a stress fracture. Now what? Getting an accurate diagnosis is essential before you decide on treatment, and there are several pathways to get there.
X-ray, CT Scan, and MRI
Most people start with an X-ray. It’s accessible, inexpensive, and quick. But here’s the frustrating part: X-rays miss stress fractures in up to 50% of early cases. Bone cracks at this stage are simply too fine to show up on standard radiographic imaging. You can walk out of an X-ray appointment feeling falsely reassured.
If clinical suspicion remains high but the X-ray is negative, an MRI is the gold standard for hairline fracture imaging. It can detect bone marrow edema, the earliest sign of a developing stress fracture, even before a visible crack forms. MRI also reveals soft tissue involvement, which helps rule out competing diagnoses.
CT scans are occasionally used when MRI isn’t available or when the fracture pattern needs more precise anatomical detail, particularly for surgical planning in complex cases.
At-Home Checks vs. Professional Evaluation
Certain self-checks, like the hop test or applying a tuning fork to the bone (vibration-induced pain at the fracture site), can raise your index of suspicion. But they are not substitutes for professional evaluation. These tools help you decide whether to see a doctor, not whether you need treatment.
A sports medicine physician or orthopedic specialist will combine your clinical history, physical examination findings, and imaging results to reach an accurate diagnosis. Don’t try to navigate this solo, especially if pain is interfering with daily activity.
Treatment Options for Stress and Hairline Fractures
Good news: most stress fractures heal well with proper management. The key word there is “proper.” Continuing to train through a stress fracture is one of the most counterproductive things you can do.
Rest, RICE Method, Crutches, and Boots
The foundation of treatment is rest. And not just “take it easy” rest, actual offloading of the injured bone. The RICE method recovery protocol (Rest, Ice, Compression, Elevation) is the starting point for managing pain and inflammation in the early phase.
For more significant fractures or those in high-risk locations, a walking boot or pneumatic brace redistributes weight away from the injured area while still allowing limited mobility. Crutches are sometimes necessary for lower extremity fractures where full weight-bearing would impede healing.
The temptation to return to activity too soon is real, especially for competitive athletes. Resist it. Premature loading is the primary reason stress fractures fail to heal properly and progress to complete breaks.
Physical Therapy and Gradual Weight Bearing
Once initial healing is underway, typically after a few weeks of rest, physical therapy becomes central to recovery. A therapist guides you through progressive weight-bearing exercises that stimulate bone remodeling without re-injuring the site. They also address the biomechanical factors that contributed to the fracture in the first place.
Strengthening the surrounding musculature reduces future mechanical stress on the bone. Gait retraining, flexibility work, and proprioceptive exercises all play a role in a comprehensive rehabilitation program. Rushing this phase is how athletes end up with repeat fractures.
Surgery and Advanced Therapies (Bone Stimulators, Ultrasound)
Surgery for hairline fracture is relatively uncommon but becomes necessary in specific scenarios: fractures in high-risk locations with poor blood supply (like the navicular), fractures that haven’t healed after extended conservative management, or cases where a full break has already occurred.
Surgical fixation typically involves inserting screws to stabilize the fracture site. Recovery post-surgery is longer but often more reliable for these complex cases.
Bone stimulator therapy uses low-level electrical or ultrasonic energy to accelerate bone repair. While not universally covered by insurance, clinical evidence supports its use in delayed healing cases. It’s non-invasive, easy to use at home, and can meaningfully reduce total recovery time in stubborn fractures.
Recovery Timeline and Healing Process
Patience is non-negotiable here. Stress fractures heal on their own schedule, and pushing that schedule is a recipe for setback.
Typical Healing Duration by Location
Metatarsal fractures generally heal in six to eight weeks with appropriate rest and immobilization. Tibial stress fractures typically require eight to twelve weeks, depending on severity and location. High-risk sites like the navicular or femoral neck may take three to six months or longer and require more aggressive management.
It’s worth noting that healing time isn’t just about the crack closing. The bone needs to fully consolidate and remodel before it can safely tolerate high-impact loading again. An X-ray showing reduced crack visibility doesn’t mean you’re ready to run a half marathon.
Monitoring Progress and Return to Activity
Progress is monitored through a combination of symptom assessment and follow-up imaging. Pain-free walking is typically the first milestone. From there, a graduated return-to-sport protocol begins, starting with low-impact activities like swimming or cycling before progressing to jogging, then running, then sport-specific training.
Any return of pain during this progression is a signal to pull back. Two steps forward, one step back is completely normal. The athletes who return successfully are the ones who respect the process.
Prevention Tips for Athletes and Active Individuals
The best fracture is the one you never get. Prevention is absolutely achievable with the right habits and awareness.
Gradual Training Increases and Cross-Training
The 10% rule is a practical starting point: don’t increase your weekly training volume by more than 10% per week. That said, it’s not a magic formula, individual factors like age, fitness level, and bone health all influence how quickly you can safely progress.
Incorporate cross-training to give your weight-bearing bones periodic relief. Swimming, cycling, and elliptical training maintain cardiovascular fitness while dramatically reducing skeletal loading. Structuring rest days strategically into your training week isn’t a sign of weakness. It’s smart periodization.
Proper Footwear and Biomechanics
Replace your running shoes every 300 to 500 miles. Most runners dramatically underestimate how quickly cushioning degrades. A worn-out shoe offers little meaningful shock absorption, effectively passing more force directly to your bones with every stride.
Get a proper gait analysis if you’re a regular runner. Overpronation, supination, and asymmetrical loading patterns all increase fracture risk and can be addressed through appropriate footwear selection or custom orthotics. These aren’t luxury interventions, they’re preventive investments.
Nutrition: Vitamin D, Calcium, and Bone Health
Your bones are only as strong as what you feed them. Vitamin D and calcium support are the two most foundational nutritional pillars of bone health. Calcium provides the structural mineral matrix of bone, while vitamin D enables its absorption. Deficiency in either accelerates bone loss and increases fracture susceptibility.
For most adults, the recommended daily calcium intake is around 1,000 mg, rising to 1,200 mg for women over 50 and men over 70. Vitamin D needs vary, but most active adults benefit from 1,500 to 2,000 IU daily. Get your levels checked through routine bloodwork, deficiency is remarkably common, even in sun-exposed populations.
Adequate protein intake matters, too. Protein supports bone remodeling and muscle recovery. Don’t neglect it in the name of weight management, particularly if you’re an endurance athlete.
When to Seek Emergency Care
Most stress fractures are not emergencies. But some presentations demand immediate attention.
Red Flags: Severe Pain, Swelling, or Numbness
If you experience sudden, severe pain following activity, especially if accompanied by rapid swelling, visible deformity, or inability to bear any weight at all, that could indicate a complete fracture rather than a stress fracture. Numbness or tingling in the foot or leg alongside bone pain can signal nerve or vascular involvement and requires urgent evaluation.
Don’t wait for a morning appointment if any of these signs appear. An emergency department visit is appropriate.
Choosing the Right Facility for Prompt Care
For most stress fracture concerns, an urgent care clinic staffed with orthopedic experience or a direct referral to a sports medicine physician is the appropriate first stop. Emergency departments are best reserved for suspected complete breaks, open fractures, or signs of neurovascular compromise.
If you’re an athlete under the care of a team physician or trainer, loop them in immediately. Early intervention is reliably better than delayed diagnosis when it comes to bone stress injuries.
FAQ’s
Will a Stress Fracture Heal on Its Own?
Yes, most stress fractures heal on their own with adequate rest and offloading of the affected bone. However, high-risk fractures in locations with poor blood supply may require surgical intervention to heal properly.
Difference Between Stress and Hairline Fractures
A stress fracture is defined by its cause, repetitive overloading of bone over time. A hairline fracture describes the physical appearance of the crack on imaging. The two terms often overlap, but they aren’t always identical in meaning.
Can It Progress to a Full Break?
Absolutely. Continuing to stress an unhealed fracture significantly increases the risk of a complete break. This is most dangerous in high-load bones like the femur or navicular. Prompt diagnosis and treatment are the best ways to prevent that progression.
FAQ’s
How long does it take for a hairline fracture in foot to heal?
Most foot hairline fractures heal within six to eight weeks with proper rest and immobilization, though high-risk locations may take longer.
Can I walk with a hairline fracture in my foot?
Limited walking in a protective boot may be permitted, but full weight-bearing activity should be avoided until your doctor confirms adequate healing progress.
Is it possible to have a stress fracture without knowing it?
Yes, early-stage stress fractures often produce mild, easy-to-dismiss symptoms. Many athletes train through them unknowingly for weeks before seeking evaluation.
Do I need surgery for a stress fracture?
Most stress fractures don’t require surgery. Surgery is typically reserved for fractures in high-risk sites, cases of failed conservative healing, or when a complete break has already occurred.
What’s the best way to prevent recurring stress fractures?
Gradual training progression, proper footwear, adequate nutrition including calcium and vitamin D, and structured rest days are the most effective strategies for preventing repeat bone stress injuries.

Liam Grant is a health writer passionate about evidence-based wellness. With a background in nutrition and digital health research, he shares practical, medically reviewed insights promoting balanced living. Evan’s work focuses on trustworthy, expert-backed health advice designed to improve daily habits, mental clarity, and overall well-being for readers worldwide.

