Have you ever felt a sharp, stabbing pain near your chest and wondered if something was seriously wrong? Maybe you dismissed it as a muscle pull or stress. But what if the real culprit was something most people have never even heard of: costal cartilage?
It sits quietly in your chest wall, doing its job every single day without any fanfare. Until it doesn’t. And when something goes wrong with it, you feel it with every single breath you take. That’s when people start asking questions they should have asked much earlier.
What Is Costal Cartilage?
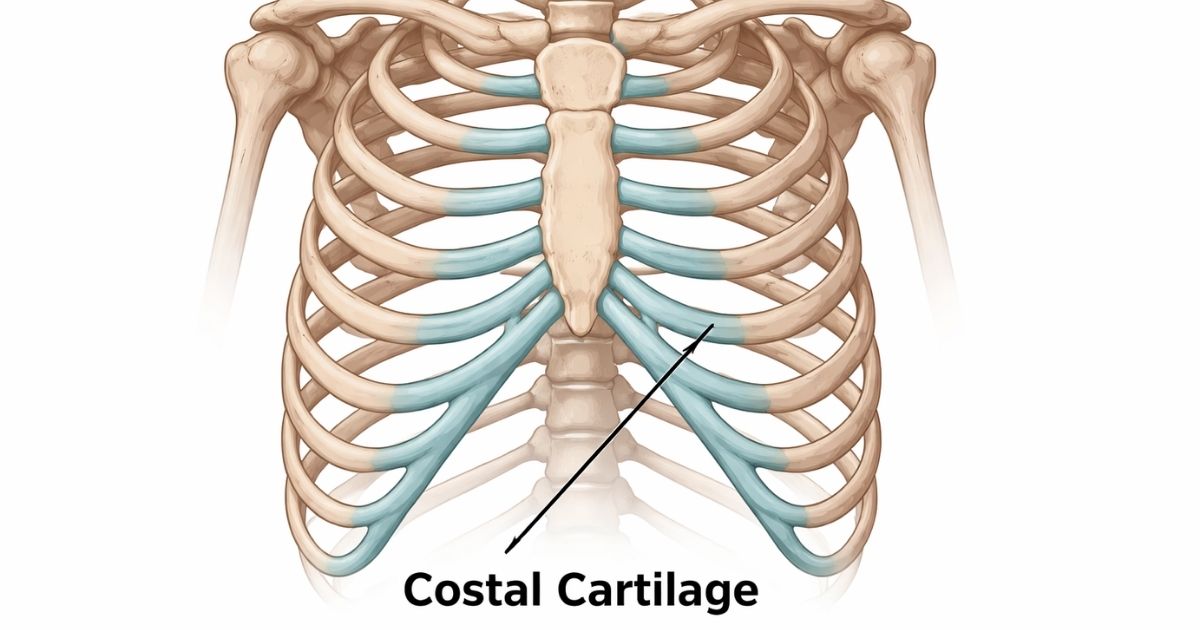
Costal cartilage is the rubbery, firm connective tissue that links your ribs to your sternum, which is the flat bone running down the center of your chest. Think of it as the flexible bridge between your rib bones and your breastbone. Without it, your rib cage would be a rigid, immovable structure. That would make breathing a real problem.
It’s made primarily of hyaline cartilage tissue, one of the most resilient cartilage types in the human body. Hyaline cartilage is smooth, pearlescent in appearance, and designed to handle repeated mechanical stress. It doesn’t have its own blood supply, which is actually why cartilage injuries tend to heal more slowly than bone fractures.
What makes costal cartilage particularly interesting is its dual role. It protects vital organs while simultaneously allowing the chest wall to expand and contract during every breath. That balance between strength and flexibility is what makes this tissue so critical.
Costal Cartilage Is Also Referred to As:
- Rib cartilage
- Anterior rib attachment tissue
- Sternal cartilage connectors
- Thoracic cartilage
These terms often pop up in clinical settings, radiology reports, or physical therapy notes. They all point to the same structure, just described from different anatomical angles.
Read More: Feel Better Fast: The Best Foods to Eat When You’re Sick
Location of Costal Cartilage
The costal cartilage is found in the anterior part of your thoracic cage, which is the front section of your rib cage. It sits between the bony portion of each rib and the sternum, acting as a natural buffer and connector.
You can actually feel it if you press gently on the lower front portion of your chest, particularly along the sides of your breastbone. That slightly firmer-yet-yielding texture under your fingers? That’s it.
Anatomical Placement of Costal Cartilage
Understanding where each piece of cartilage sits requires a quick look at how ribs are categorized. Human adults typically have 12 pairs of ribs, and they aren’t all connected in the same way.
True ribs and false ribs differ in their connection method. The first seven pairs, known as true ribs, each have their own dedicated piece of costal cartilage connecting directly to the sternum. Pairs 8 through 10 are false ribs. Their cartilage doesn’t connect to the sternum directly. Instead, it fuses with the cartilage above it, creating a shared cartilaginous arch.
Then there are floating ribs. Ribs 11 and 12 don’t connect to the sternum at all and have only a small cartilage tip at their anterior end. They literally “float” without a front attachment.
This arrangement isn’t random. It gives the lower chest more flexibility, which is especially important during deep breathing, physical exertion, and even digestion.
Costal Cartilage Function
Here’s where things get genuinely fascinating. Costal cartilage isn’t just filler between bone and bone. It plays several deeply important roles in how your body moves, breathes, and protects itself.
Primary Functions of Costal Cartilage
The first and most obvious function is structural support. It completes the front of the thoracic cage structure, giving the chest wall its characteristic shape and rigidity while still allowing movement.
The second function is respiratory flexibility. During inhalation, your diaphragm drops and your rib cage expands outward and upward. The costal cartilage allows this expansion to happen smoothly. Lung inflation and deflation depend on this elastic give. Without flexible cartilage, your chest would resist the movement your lungs need.
Third, it acts as a shock absorber. If you take a hit to the chest during sports or a fall, the cartilage distributes that force before it reaches your internal organs. It’s an underappreciated layer of protection.
Fourth, it maintains posture and structural integrity of the chest wall. When there’s a musculoskeletal imbalance, often the costal cartilage is one of the first structures affected. Pain in this area can alter your posture, your gait, and even your breathing pattern over time.
Why Understanding the Costal Cartilage Is Important?
Most people learn about costal cartilage only after something goes wrong. That’s a shame, because early awareness can prevent a lot of unnecessary pain, misdiagnosis, and anxiety.
Chest pain is one of the most alarming symptoms a person can experience. And more often than not, people immediately fear a cardiac event. In many cases though, the pain originates from the chest wall itself. Specifically, from inflamed or injured costal cartilage. Knowing the difference matters enormously.
Understanding this anatomy also helps you communicate better with your doctor. When you can describe the exact location of your pain, whether it worsens with movement, and whether pressing on your chest makes it sharper, you give clinicians useful diagnostic information. That often speeds up accurate diagnosis and appropriate treatment.
It also matters for athletes, manual laborers, and anyone with a physically demanding lifestyle. Rib cage cartilage inflammation is more common in this group than many realize. Knowing the warning signs early means you can modify activity and prevent a minor issue from becoming a prolonged injury.
How To Know That Your Costal Cartilage Pain Is Serious?
Not every chest ache is an emergency. But some signs genuinely warrant immediate attention. Learning to distinguish between the two could, in rare cases, save your life.
The tricky part is that costal cartilage pain can feel eerily similar to cardiac pain. Both can cause chest tightness, pressure, or sharp sensations. The difference is often in the details.
Common Signs of Costal Cartilage Injury
Sharp pain near the rib cage that worsens when you press on the area is one of the most telling indicators of a local cartilage issue rather than a cardiac one. Cardiac pain typically doesn’t change with palpation. If poking your chest makes it worse, that’s musculoskeletal.
Cartilage swelling symptoms include visible or palpable swelling along the rib-sternum junction. This swelling may accompany warmth and redness in the area, which are hallmarks of costochondritis inflammation. Costochondritis chest pain is one of the most common chest wall conditions, especially in people aged 20 to 40.
Pain that increases with deep breathing, twisting, or physical movement also points toward the chest wall rather than the heart. Breathing problems due to chest pain, particularly shallow breathing adopted to avoid discomfort, are a secondary but important symptom to monitor.
However, you should seek emergency chest pain evaluation immediately if you experience any of the following: chest pain radiating to your jaw, left arm, or back; sudden shortness of breath at rest; dizziness or fainting; sweating without exertion; or pain that doesn’t improve with rest or position changes. These could signal a cardiac emergency and are not symptoms to wait out.
What Causes Costal Cartilage Pain?
Costal cartilage pain doesn’t appear out of nowhere. It has identifiable triggers, and understanding them helps you both treat and prevent recurrence.
Causes of Costal Cartilage Pain
Physical trauma is the most straightforward cause. A direct blow to the chest, whether from a car accident, a sports collision, or even an intense coughing episode, can strain or fracture the cartilage. Rib cartilage injury from trauma tends to present with sharp, localized pain that worsens with movement.
Repetitive strain is another major contributor. People who lift heavy weights, row competitively, or perform repetitive upper-body movements can develop micro-tears in the cartilage over time. This is common in gym enthusiasts who ignore early warning signs and push through discomfort.
Inflammatory chest conditions, including costochondritis and Tietze syndrome, are primary medical causes. Costochondritis is diffuse inflammation without swelling, while Tietze syndrome involves localized swelling at one or two junctions. Both cause rib cage cartilage inflammation that can be debilitating during flare-ups.
Connective tissue disorders like rheumatoid arthritis, lupus, or fibromyalgia can also target costal cartilage as part of broader systemic inflammation. In these cases, the chest wall pain is one symptom among many and requires coordinated medical management.
Postural issues and thoracic health decline tied to sedentary lifestyles contribute significantly too. Prolonged sitting, hunched postures, and weak core muscles put chronic low-grade stress on the anterior chest wall. Over time, this can irritate costal cartilage and cause nagging discomfort that’s easy to dismiss until it becomes persistent.
How to Treat Costal Cartilage Injury?
The good news is that most costal cartilage injuries respond well to conservative treatment. They don’t typically require surgery unless there’s severe structural damage involved.
Rest is the first and most critical step. Continuing to strain the affected area slows healing considerably. If your injury came from sport or heavy lifting, a temporary break isn’t optional; it’s necessary. How long does costal cartilage pain last with proper rest? Mild cases often resolve within a few weeks. Moderate injuries may take 6 to 12 weeks. Severe cases or those involving connective tissue disorders can take longer and require ongoing management.
Anti-inflammatory medications are a frontline treatment option. Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen reduce both pain and inflammation. Always use them as directed and consult a healthcare provider if you need them for more than a week or two.
Topical treatments, including ice packs in the acute phase and heat therapy later in recovery, can meaningfully reduce pain and speed up tissue recovery. Applying ice for 15 to 20 minutes several times a day during the first 48 to 72 hours is a simple but effective strategy.
Corticosteroid injections are sometimes used in stubborn cases of costochondritis where oral medications haven’t provided sufficient relief. These injections are administered directly into the affected cartilage-sternum junction and can offer significant short-term pain relief.
Physical therapy plays a major role in full recovery. A therapist can work with you on breathing retraining, posture correction, and gentle mobilization techniques that reduce strain on the chest wall. This is especially important if postural imbalances or musculoskeletal dysfunction contributed to the injury in the first place.
Home remedies for costochondritis that many people find helpful include gentle stretching, diaphragmatic breathing exercises, and using supportive pillows during sleep to reduce positional pressure on the chest. These don’t replace medical care but work well as supportive measures.
When to see a doctor for chest pain: if your pain is severe, isn’t improving after two to three weeks of rest, or is accompanied by any cardiac symptoms mentioned earlier, book an appointment without delay.
Lifestyle Changes to Care About the Costal Cartilage
Prevention is always easier than treatment. A few consistent lifestyle adjustments can keep your costal cartilage healthy and reduce your risk of injury or inflammation over time.
Good posture is one of the most impactful changes you can make. Keeping your spine neutral, your shoulders back, and your chest open reduces unnecessary pressure on the anterior rib attachment area. If you work at a desk, ergonomic adjustments aren’t just about back health. They benefit your entire thoracic structure.
Avoiding sudden, jerky movements during exercise protects the cartilage from acute strain. Warming up properly before physical activity and cooling down afterward keeps the tissue supple and reduces the risk of micro-tears.
Managing underlying inflammatory conditions through medication and lifestyle is equally important. If you have a systemic inflammatory disorder, staying consistent with your treatment plan directly benefits your thoracic health care and reduces flare-up risk.
Exercises for Costal Cartilage
The best exercises for costal cartilage focus on gentle mobility and strengthening rather than aggressive loading. Deep breathing exercises, particularly diaphragmatic breathing, train your chest wall to expand fully without strain. They also improve lung capacity and reduce shallow breathing habits that often develop after an injury.
Thoracic extension stretches over a foam roller open up the chest wall and reduce stiffness around the rib-cartilage junctions. Cat-cow stretches improve spinal and thoracic mobility gently. Shoulder rolls and scapular retractions help correct the rounded posture that places chronic stress on the chest front.
Avoid any exercises that place direct pressure on the sternum or require aggressive chest compression, especially during recovery. Push-ups, heavy bench pressing, and dips should be temporarily modified or avoided entirely.
Diet for Costal Cartilage
An anti-inflammatory diet for cartilage is one of the most underutilized tools in managing costal cartilage health. What you eat directly influences how much systemic inflammation your body carries, and that inflammation is what drives much of the pain associated with cartilage conditions.
Omega-3 fatty acids found in fatty fish like salmon, mackerel, and sardines are among the most effective natural anti-inflammatory agents available. Including them regularly in your diet supports cartilage tissue health and reduces inflammatory markers across the body.
Vitamin C is essential for collagen synthesis. Since cartilage is largely composed of collagen, ensuring adequate intake through citrus fruits, bell peppers, and broccoli supports structural maintenance and repair.
Antioxidant-rich foods including berries, leafy greens, and nuts combat oxidative stress that can degrade connective tissue over time. Turmeric, ginger, and garlic have well-documented anti-inflammatory properties and work well as dietary staples rather than supplements alone.
Cutting back on processed foods, refined sugars, and excessive alcohol reduces the overall inflammatory load on your body. Small dietary shifts, done consistently, compound into meaningful protection for your cartilage over months and years.
Final Verdict: Costal Cartilage Health Starts With Early Prevention
Here’s the bottom line. Costal cartilage is a small but mighty structure. It keeps your chest wall functional, your breathing smooth, and your vital organs protected. Most people never think about it until it starts hurting. And by then, the road back to comfort takes longer than it needed to.
The smarter approach is to take it seriously before pain ever starts. Maintain good posture. Move your body thoughtfully. Eat in a way that keeps inflammation low. And if something doesn’t feel right in your chest, don’t just wait and hope it disappears. Get it checked.
Early attention to chest wall symptoms prevents misdiagnosis, reduces recovery time, and keeps small problems from becoming chronic ones. Your costal cartilage has been working hard for you every single day. Returning the favor with a bit of intentional care is the least you can do.
FAQ’s
What is costal cartilage and where is it located?
Costal cartilage is the firm, flexible tissue connecting your ribs to your sternum at the front of your chest. It sits along the anterior rib cage and is made of hyaline cartilage tissue.
What does costal cartilage pain feel like?
It typically feels like a sharp or aching pain near the sides of the breastbone that worsens with pressure, movement, or deep breathing. It often mimics cardiac pain but is localized to the chest wall.
How long does a costal cartilage injury take to heal?
Mild injuries usually recover within a few weeks with rest. More significant inflammation or trauma can take 6 to 12 weeks or longer depending on the cause and treatment approach.
Can diet help with costal cartilage inflammation?
Yes, an anti-inflammatory diet rich in omega-3s, vitamin C, and antioxidants can reduce inflammation and support cartilage repair over time. Avoiding processed foods also helps significantly.
When should you see a doctor for costal cartilage pain?
You should seek medical attention if your pain is severe, persists beyond two to three weeks, or comes with symptoms like shortness of breath, radiating pain, or dizziness, as these may indicate a more serious condition.

Liam Grant is a health writer passionate about evidence-based wellness. With a background in nutrition and digital health research, he shares practical, medically reviewed insights promoting balanced living. Evan’s work focuses on trustworthy, expert-backed health advice designed to improve daily habits, mental clarity, and overall well-being for readers worldwide.